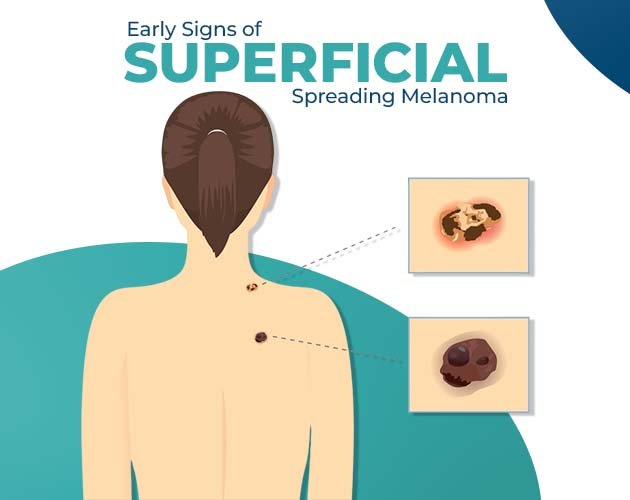
When people think of skin cancer, they often imagine an irregular, dark mole and for good reason. That classic description matches superficial melanoma, technically known as superficial spreading melanoma, which is the most common form of this potentially serious disease .
If you’ve ever wondered whether a changing mole on your skin warrants concern, understanding this specific type of melanoma is essential. Superficial spreading melanoma accounts for approximately 70% of all melanoma diagnoses . When caught early, it’s highly treatable.
This article will walk you through everything you need to know about superficial melanomafrom what it looks like and who’s at risk, to diagnosis, treatment options, and survival rates. By the end, you’ll know exactly what to watch for and when to seek medical attention.
What Is Superficial Melanoma?
“Superficial spreading melanoma is a type of skin cancer that begins in the melanocytes the cells that produce the skin-darkening pigment melanin . What makes this particular melanoma unique is its growth pattern.”
As the name suggests, superficial spreading melanoma initially grows horizontally across the top layer of skin (the epidermis). This phase is called radial growth . During this time, the cancer remains on the skin’s surface and may stay there for months, years, or even decades before penetrating deeper .
If left untreated, it can eventually grow vertically into the deeper layers of skin (the dermis). Once this happens, it becomes invasive melanoma, which has the potential to spread to lymph nodes and other organs .
Superficial Melanoma vs. Melanoma in Situ
When the cancerous cells remain entirely within the epidermis meaning they haven’t invaded deeper layers this is known as melanoma in situ . At this stage, the melanoma is considered stage 0 and is 100% curable with complete surgical removal .
The Key Difference from Other Melanomas
Unlike nodular melanoma, which grows aggressively downward from the start, superficial spreading melanoma’s slow, outward growth pattern provides a crucial window for early detection and treatment . This is why regular skin checks are so important you have time to spot it before it becomes dangerous.
How Common Is Superficial Spreading Melanoma?
Superficial spreading melanoma is by far the most common type of melanoma, accounting for approximately 70% of all cases .
Here’s what the statistics tell us:
- Age distribution: While it can occur in adults of all ages, it’s most common in people over 40. Only about 15% of cases arise under age 40, and less than 1% occur in people under 20 .
- Gender differences: It affects both men and women, but location varies. In men, it’s most common on the head, neck, and torso. In women, it occurs more often on the legs and feet .
- Skin tone: This type of melanoma almost always occurs in light-skinned individuals as a result of sun exposure . However, people of all skin tones can develop melanoma, just usually different types.
How Does Superficial Melanoma Look Like?
Recognizing superficial spreading melanoma starts with knowing what to look for. These lesions can appear anywhere on the body, either as a new mole or as changes within an existing mole .
The Classic Appearance
Superficial spreading melanomas typically appear as:
- A flat or slightly raised patch on the skin
- Irregular or asymmetrical shape (one half doesn’t match the other)
- Uneven borders that may be notched, ragged, or blurred
- Multiple colors within the same lesion light brown, dark brown, black, red, pink, blue, or even white
- Usually larger than 6 millimeters across (about the size of a pencil eraser), though they can be smaller
The ABCDE Method for Detection
The ABCDE rule is a simple way to remember what to check for :
| Letter | Meaning | What to Look For |
|---|---|---|
| A | Asymmetry | One half doesn’t match the other half |
| B | Border | Edges are irregular, ragged, notched, or blurred |
| C | Color | Uneven coloring with shades of brown, black, tan, red, white, or blue |
| D | Diameter | Larger than 6mm (pencil eraser size), though melanomas can be smaller |
| E | Evolving | Changing in size, shape, or color, or new symptoms like bleeding or itching |
The Ugly Duckling Sign
Another helpful approach is the “ugly duckling” method. Most of your normal moles resemble each other they look like a matching set. If you have one spot that looks completely different from your other moles, that’s the “ugly duckling” worth having checked .
Beyond the ABCDEs
Some superficial spreading melanomas may also:
- Feel different in texture from surrounding skin
- Develop a dark, raised nodule within the flat patch
- Bleed or ooze spontaneously
- Appear as a mole that looks like it’s spreading beyond its original borders
Important Caveat
Not all superficial spreading melanomas follow these rules perfectly. Some may be smaller than 6mm or have more subtle features. When in doubt, get it checked out .
What Causes Superficial Melanoma?
Superficial spreading melanoma develops when DNA mutations occur in melanocytes, causing them to grow uncontrollably . While the exact trigger for these mutations isn’t always clear, researchers have identified several key risk factors.
Ultraviolet (UV) Exposure: The Primary Culprit
UV radiation from sunlight and tanning beds is the primary risk factor for superficial spreading melanoma . However, it’s not just about total lifetime exposure the pattern of exposure matters.
- Intermittent intense exposure (like weekend sunbathing or vacations) appears more dangerous than steady, moderate exposure
- History of sunburn, especially blistering sunburns in childhood, significantly increases risk
- Tanning bed use is particularly harmful, especially with 10 or more sessions
Personal Characteristics
Your natural traits also play a major role :
- Fair skin that burns rather than tans (Fitzpatrick skin types I and II)
- Red or blonde hair
- Blue or green eyes
- Numerous moles having 50 or more moles, or 5 or more atypical moles
- Freckles, especially on the upper back
- Increasing age, with highest rates in people over 50
Medical and Family History
- Personal history of melanoma or other skin cancers
- Family history of melanoma in a first-degree relative (parent, sibling, or child)
- Weakened immune system from medications or medical conditions
How Is Superficial Melanoma Diagnosed?
If you notice a suspicious spot, here’s what you can expect during the diagnostic process.
Clinical Examination
Your doctor or dermatologist will first examine the area, often using a dermatoscope a special magnifying lens with a light that allows them to see structures in the skin invisible to the naked eye . They’ll look for features like asymmetric structures, multiple colors, and atypical pigment networks.
Biopsy: The Gold Standard
If the lesion looks suspicious, the next step is a biopsy . This involves removing the tissue for laboratory examination.
For suspected melanoma, an excisional biopsy is preferred removing the entire lesion along with a small margin of healthy tissue . This provides the pathologist with the complete picture needed for accurate diagnosis.
Pathology Report
A pathologist examines the tissue under a microscope and provides a report that includes:
- Confirmation of whether cancer cells are present
- Breslow thickness a vertical measurement in millimeters from the top of the lesion to its deepest point . This is the single most important factor in determining prognosis and treatment .
- Ulceration status (whether the skin surface is broken)
- Mitotic rate (how fast cells are dividing)
Staging and Further Testing
If the melanoma is deeper than 1mm or has other concerning features, your doctor may recommend :
- Sentinel lymph node biopsy to check if cancer has spread to nearby lymph nodes
- Imaging tests (CT scans, MRIs, or PET scans) if there’s concern about distant spread
Melanoma Stages at a Glance
| Stage | Description | 5-Year Survival Rate |
|---|---|---|
| Stage 0 | Melanoma in situ (confined to epidermis) | 100% |
| Stage I-II | Localized to skin, no spread | 97.6% |
| Stage III | Spread to nearby lymph nodes | 60.3% |
| Stage IV | Spread to distant organs | 16.2% |
Treatment Options for Superficial Melanoma
Treatment depends primarily on the stage and Breslow thickness of the melanoma.
Surgery: The Primary Treatment
For early-stage superficial spreading melanoma, surgical excision is both diagnostic and curative .
- Wide local excision removes the melanoma along with a margin of healthy skin. The margin size is determined by the tumor’s thickness :
- Thin melanomas: 1cm margin
- Thicker melanomas: 2cm margin
Treatment for Advanced Disease
If the melanoma has spread beyond the skin, additional treatments may be necessary :
- Immunotherapy: Medications that help your immune system recognize and attack cancer cells. Used for advanced stages or more aggressive melanomas .
- Targeted therapy: For melanomas with specific gene mutations (like BRAF), drugs can block the pathways that allow cancer to grow. BRAF mutations are more common in superficial spreading melanoma .
- Radiation therapy: High-energy rays that damage cancer cells’ DNA .
- Chemotherapy: Anti-cancer medications, typically used when other treatments aren’t effective .
- Clinical trials: Many new treatments are being studied; ask your doctor if a trial might be right for you .
Survival Rate and Prognosis
The outlook for superficial spreading melanoma is excellent when caught early.
Overall Survival Statistics
A large study of nearly 100,000 superficial spreading melanoma cases found an overall survival rate of 95% . This high rate reflects the slow-growing nature of this melanoma type and the effectiveness of early treatment.
What Affects Prognosis?
Several factors influence outcomes :
- Tumor thickness This is the most important factor. Thinner tumors have much better outcomes.
- Ulceration Melanomas with ulcerated surfaces have a worse prognosis.
- Location Melanomas on arms or legs may have better outcomes than those on the head, neck, or trunk.
- Age and gender Younger patients and females tend to have better outcomes.
- Spread Whether cancer has reached lymph nodes or distant organs.
Recurrence Risk
Even after successful treatment, about 5-10% of melanoma patients will experience a recurrence . Additionally, more than 20% will develop a new, unrelated melanoma (melanoma in situ) . This is why ongoing skin surveillance is essential.
Prevention and Early Detection Strategies
You can significantly reduce your risk of superficial spreading melanoma through simple, consistent habits.
Sun Safety Practices
- Use SPF 50+ sunscreen broad-spectrum, water-resistant, applied 30 minutes before going out and reapplied every 2 hours
- Wear protective clothing including wide-brimmed hats, long sleeves, and sunglasses
- Seek shade during peak UV hours (10 a.m. to 4 p.m.)
- Avoid tanning beds completely use sunless tanning products if you want a tan appearance
- Check medications with your doctor some can increase sun sensitivity
Regular Skin Checks
- Monthly self-exams: Use a full-length mirror and hand-held mirror to check all areas, including your back, scalp, and between toes. Have someone help with hard-to-see areas .
- Professional skin checks: Yearly exams by a dermatologist or trained professional, more frequently if you have risk factors .
Know Your Skin
Familiarize yourself with your moles and spots so you can recognize changes quickly. If something is new, changing, or just looks “off” trust your instincts and get it checked.
Pros and Cons of Early Detection
Pros of Early Detection
- Cure rates approach 100% for stage 0 melanoma
- Minimally invasive treatment simple outpatient surgery
- Lower healthcare costs compared to advanced cancer treatment
- No need for chemotherapy, radiation, or immunotherapy
- Peace of mind knowing you’ve addressed the issue
Cons of Late Diagnosis
- More extensive surgery with larger margins
- Potential lymph node involvement requiring additional procedures
- Need for adjuvant therapies like immunotherapy
- Lower survival rates stage IV survival drops to 16.2%
- Ongoing surveillance and anxiety about recurrence
Frequently Asked Questions
How fast does superficial spreading melanoma grow?
Superficial spreading melanoma grows slowly compared to other types like nodular melanoma. The median growth rate is approximately 0.12 mm per month . It can remain in the horizontal growth phase for months to years or even decades before becoming invasive .
Can superficial spreading melanoma be completely cured?
Yes, absolutely especially when caught early. Stage 0 melanoma (in situ) has a 100% cure rate with complete surgical excision . Even early-stage invasive melanoma has excellent outcomes, with 97.6% 5-year survival for localized disease.
Does superficial spreading melanoma always start from an existing mole?
No. While about 25% of cases arise from an existing mole, the majority approximately 75% develop as a new lesion on normal-looking skin . This is why monitoring for any new or changing spot is important, not just existing moles.
What’s the difference between superficial spreading melanoma and nodular melanoma?
A: The main difference is growth pattern. Superficial spreading melanoma grows outward across the skin surface first, remaining flat for some time. Nodular melanoma grows downward into deeper skin layers from the start, making it more aggressive and harder to detect early