Do you feel exhausted after a full night’s sleep? Are you struggling to concentrate, feeling short of breath after a short walk, or looking paler than usual? You might be experiencing the silent and often misunderstood symptoms of iron deficiency.
Iron is the engine behind your red blood cells, carrying oxygen to every part of your body. When levels drop, your entire system feels the strain. But here’s the challenge: diagnosing iron deficiency isn’t always straightforward. Symptoms can be vague, and the condition often goes unnoticed until it progresses to anemia.
This is where the Iron Deficiency Calculator by MedTree comes in. Designed as a preliminary screening tool, this calculator helps you understand your risk level based on key symptoms and personal factors. In this article, we will explore how iron deficiency affects the body, how the calculator works, and the next steps you should take to reclaim your vitality.
What is Iron Deficiency?
Iron deficiency is a condition where your body lacks sufficient iron to maintain normal physiological functions. It is the most common nutritional deficiency worldwide, affecting an estimated 25% of the global population .
The Stages of Iron Deficiency
Iron deficiency is not an all-or-nothing condition; it progresses through stages:
- Mild Iron Deficiency (Iron Depletion): Iron stores in the bone marrow are low, but hemoglobin levels remain normal. You may feel slightly tired or have no symptoms at all.
- Iron-Deficiency Erythropoiesis: The body struggles to produce red blood cells due to insufficient iron. Fatigue becomes more noticeable.
- Iron Deficiency Anemia (IDA): This is the most severe stage. Hemoglobin levels drop below the normal range, leading to classic anemia symptoms like pale skin, extreme fatigue, and shortness of breath.
Why is Iron So Vital?
Iron is the core component of hemoglobin—the protein in red blood cells that carries oxygen from your lungs to your tissues. Without enough iron, your organs and muscles literally starve for oxygen, leading to the cascade of symptoms associated with the condition.
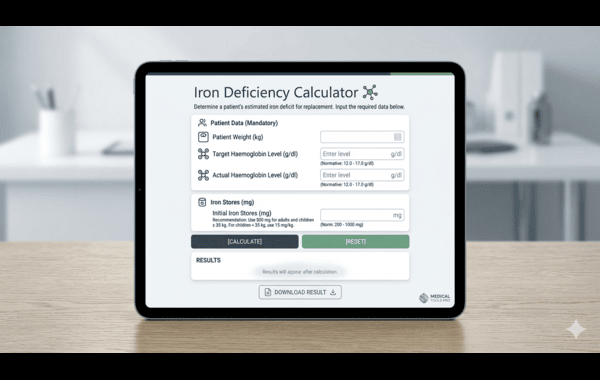
Introducing the Iron Deficiency Calculator by MedTree
The Iron Deficiency Calculator is a digital screening tool developed to help individuals assess their likelihood of having low iron levels before they visit a doctor.
How It Works?
The calculator uses a probabilistic algorithm based on medical guidelines. It asks a series of questions regarding:
- Demographics: Age, gender, and life stage (pregnancy status).
- Dietary Intake: Consumption of iron-rich foods (red meat, leafy greens) or inhibitors (excessive tea/coffee with meals).
- Clinical Symptoms: Presence of fatigue, pallor, shortness of breath, and restless legs.
- Risk Factors: History of heavy menstrual bleeding, gastrointestinal disorders (like celiac or Crohn’s disease), or recent surgery.
Based on your inputs, the tool generates a risk score (e.g., Low, Moderate, or High) and provides a summary of findings.
The Technology Behind the Tool
The MedTree calculator leverages clinical guidelines from organizations like the World Health Organization (WHO) and the American Gastroenterological Association (AGA) . It cross-references user-reported data with statistical models used in primary care settings to triage patients.
How to Use the Iron Deficiency Calculator? (Step-by-Step)
Using the calculator is designed to be simple and user-friendly, taking less than 3 minutes.
- Visit the MedTree Health Tools Section: Navigate to the MedTree platform where the calculator is hosted.
- Input Basic Information: Enter your age, sex, and whether you are currently pregnant (if applicable).
- Symptom Checker: Select the symptoms you are experiencing from a list, such as:
- Chronic fatigue
- Cold hands and feet
- Brittle nails or spoon-shaped nails (koilonychia)
- Pica (cravings for ice, dirt, or starch)
- Medical History: Indicate if you have conditions known to cause malabsorption (like Crohn’s disease) or chronic blood loss (like heavy menstruation or ulcers).
- Dietary Assessment: Note your typical intake of iron and foods that inhibit absorption.
- Receive Your Results: The system will generate a risk assessment and recommend whether a full blood count (FBC) and iron studies are warranted.
Important Disclaimer: The Iron Deficiency Calculator is a screening tool, not a diagnostic device. It cannot replace a formal blood test or a consultation with a healthcare professional.
Common Causes of Iron Deficiency
To interpret the results of your calculator assessment, it helps to understand the root causes.
1. Blood Loss (The Most Common Cause)
- Women: Heavy menstrual bleeding (menorrhagia) is the leading cause in premenopausal women.
- Gastrointestinal: Slow, chronic bleeding from ulcers, polyps, or colon cancer.
- Medications: Regular use of aspirin or NSAIDs (like ibuprofen) can cause gastrointestinal bleeding.
2. Lack of Iron in the Diet
- Vegetarian/Vegan Diets: Non-heme iron (from plants) is less easily absorbed than heme iron (from meat).
- Poor Absorption: Conditions like celiac disease, gastric bypass surgery, or H. pylori infection prevent the body from absorbing iron, even if you eat enough.
3. Increased Need
- Pregnancy: The body needs significantly more iron to expand blood volume and support the fetus.
- Infancy and Adolescence: Rapid growth spurts require substantial iron stores.
Symptoms That Trigger a “High Risk” Score
If you input the following into the calculator, you will likely receive a high-risk result and a recommendation to see a doctor immediately:
- Extreme Fatigue: Inability to perform daily tasks.
- Pica: Unusual cravings for non-food items (ice, clay, paper).
- Pallor: Visible paleness in the face, inner eyelids, or nail beds.
- Tachycardia: Heart palpitations or a racing heart.
- Shortness of Breath: Even during light physical activity.
Pros and Cons of Using an Iron Deficiency Calculator
Pros
- Accessibility: Available 24/7, allowing users to assess risk from the comfort of home.
- Awareness: Helps demystify vague symptoms, prompting users to take fatigue seriously.
- Time-Efficient: Provides instant feedback without waiting for a doctor’s appointment.
- Data-Driven: Encourages users to gather their symptoms and history before seeing a GP, making the clinical visit more productive.
Cons
- Not Diagnostic: It cannot measure actual ferritin or hemoglobin levels; it only assesses risk based on user-reported data.
- False Sense of Security: A “low risk” result might delay a user from seeking help for other underlying conditions that mimic iron deficiency (e.g., hypothyroidism, chronic fatigue syndrome).
- Subjectivity: Symptoms like “fatigue” are subjective. The calculator relies on the user’s honesty and self-awareness.
- Technical Limitations: It cannot account for complex medical interactions without a physical examination.
Frequently Asked Questions
Q1: Is the Iron Deficiency Calculator by MedTree accurate?
The calculator is based on established clinical guidelines and epidemiological data. However, it is a screening tool. It is highly accurate at identifying risk patterns, but only a blood test (specifically a serum ferritin test) can definitively diagnose iron deficiency.
Q2: What is the difference between iron deficiency and anemia?
Iron deficiency means your body’s iron stores are low. Anemia means your red blood cell count or hemoglobin is low. Iron deficiency often leads to anemia, but you can be iron deficient without being anemic. The calculator screens for deficiency risk, not just anemia.
Q3: What should I do if I get a “High Risk” result?
If the calculator indicates high risk, you should:
- Book an appointment with your general practitioner.
- Request a Full Blood Count (FBC) and Iron Studies (including ferritin, transferrin saturation).
- Do not start iron supplements until a doctor confirms deficiency, as excess iron can be toxic.
Q4: Can I use this calculator if I am pregnant?
Yes. Pregnancy significantly increases iron requirements. The calculator includes pregnancy as a specific variable to adjust the risk algorithm accordingly. However, all pregnant women should have their iron levels checked routinely by their obstetrician or midwife.
Q5: What are the best dietary sources of iron?
- Heme Iron (Best Absorption): Red meat, liver, poultry, and fish.
- Non-Heme Iron: Spinach, lentils, beans, tofu, and fortified cereals.
- Enhancers: Vitamin C (citrus fruits) helps absorption.
- Inhibitors: Calcium and tannins (tea/coffee) reduce absorption if consumed with meals.
Q6: How long does it take to fix iron deficiency?
If you are taking supplements (ferrous sulfate), you may feel better in 2 to 4 weeks, but it can take 3 to 6 months to fully restore iron stores. The calculator helps you understand the need for consistency in treatment.
Beyond the Calculator: Diagnosis and Treatment
If the Iron Deficiency Calculator indicates moderate or high risk, and your subsequent blood work confirms low ferritin, your doctor will discuss treatment options.
1. Oral Iron Supplements
- Standard: Ferrous sulfate (325 mg).
- Side Effects: Constipation, nausea, dark stools.
- Best Practice: Take on an empty stomach with vitamin C (orange juice) for maximum absorption.
2. Intravenous (IV) Iron
Reserved for patients who:
- Cannot tolerate oral supplements.
- Have malabsorption issues (e.g., after gastric bypass).
- Need rapid replenishment (e.g., late-stage pregnancy).
3. Addressing the Root Cause
Treating the symptoms is not enough. A good doctor will also investigate why you are losing iron. This may involve:
- Gynecological evaluation for heavy periods.
- Gastroenterology referral for colonoscopy/endoscopy to rule out internal bleeding.
Why MedTree? Expertise and Trust
MedTree is a reputable health informatics platform dedicated to bridging the gap between patients and clinical care. The Iron Deficiency Calculator was developed with input from hematologists and general practitioners to ensure the tool aligns with modern medical standards.
Conclusion
Iron deficiency is a silent drain on your quality of life. It robs you of energy, clouds your thinking, and strains your heart. The Iron Deficiency Calculator by MedTree offers a simple, immediate way to understand your risk and stop guessing about your symptoms.